13 results
Geometric vertex decomposition and liaison
- Part of
- Patricia Klein, Jenna Rajchgot
-
- Journal:
- Forum of Mathematics, Sigma / Volume 9 / 2021
- Published online by Cambridge University Press:
- 19 October 2021, e70
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Geometric vertex decomposition and liaison are two frameworks that have been used to produce similar results about similar families of algebraic varieties. In this paper, we establish an explicit connection between these approaches. In particular, we show that each geometrically vertex decomposable ideal is linked by a sequence of elementary G-biliaisons of height
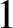 $1$ to an ideal of indeterminates and, conversely, that every G-biliaison of a certain type gives rise to a geometric vertex decomposition. As a consequence, we can immediately conclude that several well-known families of ideals are glicci, including Schubert determinantal ideals, defining ideals of varieties of complexes and defining ideals of graded lower bound cluster algebras.
$1$ to an ideal of indeterminates and, conversely, that every G-biliaison of a certain type gives rise to a geometric vertex decomposition. As a consequence, we can immediately conclude that several well-known families of ideals are glicci, including Schubert determinantal ideals, defining ideals of varieties of complexes and defining ideals of graded lower bound cluster algebras.
Pediatric surgical site infection (SSI) following ambulatory surgery: Incidence, risk factors and patient outcomes
- Michael L. Rinke, David G. Bundy, Moonseong Heo, Lisa Saiman, Barbara Rabin, Philip Zachariah, Rebecca E. Rosenberg, Patricia DeLaMora, Parsa Mirhaji, Michael Drasher, Elizabeth Klein, Oghale Obaro-Best, William J.H. Ford, Diana Zarowin, Alexandre Peshansky, Suzette O. Oyeku
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 8 / August 2022
- Published online by Cambridge University Press:
- 11 August 2021, pp. 1036-1042
- Print publication:
- August 2022
-
- Article
- Export citation
-
Background:
Inpatient surgical site infections (SSIs) cause morbidity in children. The SSI rate among pediatric ambulatory surgery patients is less clear. To fill this gap, we conducted a multiple-institution, retrospective epidemiologic study to identify incidence, risk factors, and outcomes.
Methods:We identified patients aged <22 years with ambulatory visits between October 2010 and September 2015 via electronic queries at 3 medical centers. We performed sample chart reviews to confirm ambulatory surgery and adjudicate SSIs. Weighted Poisson incidence rates were calculated. Separately, we used case–control methodology using multivariate backward logistical regression to assess risk-factor association with SSI.
Results:In total, 65,056 patients were identified by queries, and we performed complete chart reviews for 13,795 patients; we identified 45 SSIs following ambulatory surgery. The weighted SSI incidence following pediatric ambulatory surgery was 2.00 SSI per 1,000 ambulatory surgeries (95% confidence interval [CI], 1.37–3.00). Integumentary surgeries had the highest weighted SSI incidence, 3.24 per 1,000 ambulatory surgeries (95% CI, 0.32–12). The following variables carried significantly increased odds of infection: clean contaminated or contaminated wound class compared to clean (odds ratio [OR], 9.8; 95% CI, 2.0–48), other insurance type compared to private (OR, 4.0; 95% CI, 1.6–9.8), and surgery on weekend day compared to weekday (OR, 30; 95% CI, 2.9–315). Of the 45 instances of SSI following pediatric ambulatory surgery, 40% of patients were admitted to the hospital and 36% required a new operative procedure or bedside incision and drainage.
Conclusions:Our findings suggest that morbidity is associated with SSI following ambulatory surgery in children, and we also identified possible targets for intervention.
Predicting Vancomycin-Resistant Enterococci (VRE) and Carbapenem-Resistant Organism (CRO) Colonization in the Intensive Care Unit
- Çaǧlar Çaǧlayan, Scott Levin, Aaron Michael Milstone, Pranita Tamma, Patricia Simner, Katherine Goodman, Joe Amoah, Aria Smith, Matt Toerper, Sean Barnes, Eili Klein
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s45
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Rapidly identifying patients colonized with multidrug-resistant organisms (MDROs) upon ICU admission is critical to control and prevent the spread of these pathogens in healthcare facilities. Electronic health records (EHR) provide a rich source of data to predict the likelihood of MDRO colonization at admission, whereas surveillance methods are resource intensive and results are not immediately available. Our objectives were (1) to predict VRE and CRO colonization at ICU admission and (2) to identify patient subpopulations at higher risk for colonization with these MDROs. Methods: We conducted a retrospective analysis of patients aged ≥16 years admitted to any of 6 medical or surgical intensive care units (ICU) in the Johns Hopkins Hospital from July 1, 2016, through June 30, 2018. Perirectal swabs were collected at ICU unit admission and were tested for VRE and CRO. Patient demographic data, prior hospitalizations, and preadmission clinical data, including prior medication administration, prior diagnoses, and prior procedures, were extracted to develop prediction models. We employed the machine-learning algorithms logistic regression (LR), random forest (RF), and XGBoost (XG). The sum of sensitivity and specificity (ie, Youden’s index) was selected as the performance metric. Results: In total, 5,033 separate ICU visits from 3,385 patients were included, where 555 (11%) and 373 (7%) admissions tested positive for VRE and CRO, respectively. The sensitivity and specificity of our models for VRE were 78% and 80% with LR, 80% and 82% with RF, and 77% and 87% with XG. Predictions for CRO were not as precise, with LR at 73% and 53%, RF at 81% and 48%, and XG at 69% and 61%. The XG algorithm was the best-performing algorithm for both VRE and CRO. Prior VRE colonization, recent (<180 days) long-term care facility stay, and prior hospitalization >60 days were the key predictors for VRE, whereas the primary predictor for CRO colonization was prior carbapenem use. Conclusions: We demonstrated that EHR data can be used to predict >75% of VRE positive cases with a <15% false-positive rate and ~70% of CRO cases with a <40% false-positive rate. Future studies using larger sample sizes may improve the prediction accuracy and inform model generalizability across sites and thus reduce the risk of transmission of MDROs by rapidly identifying MDRO-colonized patients.
Funding: This work was funded by the Centers for Disease Control and Prevention (CDC) Epicenters Program (Grant Number 1U54CK000447) and the CDC MInD-Healthcare Program (Grant Number 1U01CK000536).
Disclosures: Aaron Milstone, BD (consulting)
Costs of ambulatory pediatric healthcare-associated infections: Central-line–associated bloodstream infection (CLABSIs), catheter-associated urinary tract infection (CAUTIs), and surgical site infections (SSIs)
- Michael L. Rinke, Suzette O. Oyeku, William J. H. Ford, Moonseong Heo, Lisa Saiman, Patricia DeLaMora, Barbara Rabin, Philip Zachariah, Rebecca E. Rosenberg, Parsa Mirhaji, Oghale Obaro-Best, Michael Drasher, Elizabeth Klein, Alexandre Peshansky, David G. Bundy
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 11 / November 2020
- Published online by Cambridge University Press:
- 03 September 2020, pp. 1292-1297
- Print publication:
- November 2020
-
- Article
- Export citation
-
Objective:
Ambulatory healthcare-associated infections (HAIs) occur frequently in children and are associated with morbidity. Less is known about ambulatory HAI costs. This study estimated additional costs associated with pediatric ambulatory central-line–associated bloodstream infections (CLABSIs), catheter-associated urinary tract infections (CAUTI), and surgical site infections (SSIs) following ambulatory surgery.
Design:Retrospective case-control study.
Setting:Four academic medical centers.
Patients:Children aged 0–22 years seen between 2010 and 2015 and at risk for HAI as identified by electronic queries.
Methods:Chart review adjudicated HAIs. Charges were obtained for patients with HAIs and matched controls 30 days before HAI, on the day of, and 30 days after HAI. Charges were converted to costs and 2015 USD. Mixed-effects linear regression was used to estimate the difference-in-differences of HAI case versus control costs in 2 models: unrecorded charge values considered missing and a sensitivity analysis with unrecorded charge considered $0.
Results:Our search identified 177 patients with ambulatory CLABSIs, 53 with ambulatory CAUTIs, and 26 with SSIs following ambulatory surgery who were matched with 382, 110, and 75 controls, respectively. Additional cost associated with an ambulatory CLABSI was $5,684 (95% confidence interval [CI], $1,005–$10,362) and $6,502 (95% CI, $2,261–$10,744) in the 2 models; cost associated with a CAUTI was $6,660 (95% CI, $1,055, $12,145) and $2,661 (95% CI, −$431 to $5,753); cost associated with an SSI following ambulatory surgery at 1 institution only was $6,370 (95% CI, $4,022–$8,719).
Conclusions:Ambulatory HAI in pediatric patients are associated with significant additional costs. Further work is needed to reduce ambulatory HAIs.
Pediatric ambulatory catheter-associated urinary tract infections (CAUTIs): Incidence, risk factors, and patient outcomes
- Michael L. Rinke, Suzette O. Oyeku, Moonseong Heo, Lisa Saiman, Philip Zachariah, Rebecca E. Rosenberg, Patricia DeLaMora, Barbara Rabin, Parsa Mirhaji, Elizabeth Klein, William J. H. Ford, Oghale Obaro-Best, Michael Drasher, Alexandre Peshansky, Kelly Ann Balem, David G. Bundy
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 8 / August 2020
- Published online by Cambridge University Press:
- 05 June 2020, pp. 891-899
- Print publication:
- August 2020
-
- Article
- Export citation
-
Objective:
Catheter-associated urinary tract infections (CAUTIs) occur frequently in pediatric inpatients, and they are associated with increased morbidity and cost. Few studies have investigated ambulatory CAUTIs, despite at-risk children utilizing home urinary catheterization. This retrospective cohort and case-control study determined incidence, risk factors, and outcomes of pediatric patients with ambulatory CAUTI.
Design:Broad electronic queries identified potential patients with ambulatory urinary catheters, and direct chart review confirmed catheters and adjudicated whether ambulatory CAUTI occurred. CAUTI definitions included clean intermittent catheterization (CIC). Our matched case-control analysis assessed risk factors.
Setting:Five urban, academic medical centers, part of the New York City Clinical Data Research Network.
Patients:Potential patients were age <22 years who were seen between October 2010 and September 2015.
Results:In total, 3,598 eligible patients were identified; 359 of these used ambulatory catheterization (representing186,616 ambulatory catheter days). Of these, 63 patients (18%) experienced 95 ambulatory CAUTIs. The overall ambulatory CAUTI incidence was 0.51 infections per 1,000 catheter days (1.35 for indwelling catheters and 0.47 for CIC; incidence rate ratio, 2.88). Patients with nonprivate medical insurance (odds ratio, 2.5; 95% confidence interval, 1.1–6.3) were significantly more likely to have ambulatory CAUTIs in bivariate models but not multivariable models. Also, 45% of ambulatory CAUTI resulted in hospitalization (median duration, 3 days); 5% resulted in intensive care admission; 47% underwent imaging; and 88% were treated with antibiotics.
Conclusions:Pediatric ambulatory CAUTIs occur in 18% of patients with catheters; they are associated with morbidity and healthcare utilization. Ambulatory indwelling catheter CAUTI incidence exceeded national inpatient incidence. Future quality improvement research to reduce these harmful infections is warranted.
The impact of maternal periodontitis in the development of asthma in the offspring
- Grazielle Rodrigues, Alexandre do Valle Wuo, Simone Klein, Patrícia de Almeida, Amilcar Sabino Damazo, Rodrigo Labat Marcos, Anna Carolina Ratto Tempestini Horliana, Adriana Lino-dos-Santos-Franco
-
- Journal:
- Journal of Developmental Origins of Health and Disease / Volume 12 / Issue 2 / April 2021
- Published online by Cambridge University Press:
- 21 April 2020, pp. 293-299
-
- Article
- Export citation
-
Clinical and experimental studies show an association between maternal periodontitis and adverse outcomes during gestation. On the other hand, there were no studies evaluating the impact of maternal periodontitis on the offspring. Thus, our objective was to investigate the repercussion of maternal periodontitis on the development of asthma in the offspring. Pregnant rats were submitted or not to periodontitis by ligature technique. Thirty days after birth, the puppies were sensitized and challenged with ovalbumin (OVA) in order to induce asthmatic response. Our results showed that maternal periodontitis reduced cellular infiltrate in the parenchyma of offspring, tracheal responsiveness, lung edema, and anti-OVA antibodies, without alter mucus as well as cytokines production. We concluded that periodontitis has relevant impact on the offspring’s immune system, blunting the response to allergic and inflammatory stimulus. This study shows the important role of oral health during pregnancy and opens possibilities for future studies in order to explain the effects of periodontitis during pregnancy in the offspring.
Predicting probability of perirectal colonization with carbapenem-resistant Enterobacteriaceae (CRE) and other carbapenem-resistant organisms (CROs) at hospital unit admission
- Katherine E. Goodman, Patricia J. Simner, Eili Y. Klein, Abida Q. Kazmi, Avinash Gadala, Matthew F. Toerper, Scott Levin, Pranita D. Tamma, Clare Rock, Sara E. Cosgrove, Lisa L. Maragakis, Aaron M. Milstone, for the CDC Prevention Epicenters Program, the CDC MIND-Healthcare Program
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 40 / Issue 5 / May 2019
- Published online by Cambridge University Press:
- 27 March 2019, pp. 541-550
- Print publication:
- May 2019
-
- Article
- Export citation
-
Background:
Targeted screening for carbapenem-resistant organisms (CROs), including carbapenem-resistant Enterobacteriaceae (CRE) and carbapenemase-producing organisms (CPOs), remains limited; recent data suggest that existing policies miss many carriers.
Objective:Our objective was to measure the prevalence of CRO and CPO perirectal colonization at hospital unit admission and to use machine learning methods to predict probability of CRO and/or CPO carriage.
Methods:We performed an observational cohort study of all patients admitted to the medical intensive care unit (MICU) or solid organ transplant (SOT) unit at The Johns Hopkins Hospital between July 1, 2016 and July 1, 2017. Admission perirectal swabs were screened for CROs and CPOs. More than 125 variables capturing preadmission clinical and demographic characteristics were collected from the electronic medical record (EMR) system. We developed models to predict colonization probabilities using decision tree learning.
Results:Evaluating 2,878 admission swabs from 2,165 patients, we found that 7.5% and 1.3% of swabs were CRO and CPO positive, respectively. Organism and carbapenemase diversity among CPO isolates was high. Despite including many characteristics commonly associated with CRO/CPO carriage or infection, overall, decision tree models poorly predicted CRO and CPO colonization (C statistics, 0.57 and 0.58, respectively). In subgroup analyses, however, models did accurately identify patients with recent CRO-positive cultures who use proton-pump inhibitors as having a high likelihood of CRO colonization.
Conclusions:In this inpatient population, CRO carriage was infrequent but was higher than previously published estimates. Despite including many variables associated with CRO/CPO carriage, models poorly predicted colonization status, likely due to significant host and organism heterogeneity.
How frequently are hospitalized patients colonized with carbapenem-resistant Enterobacteriaceae (CRE) already on contact precautions for other indications?
- Katherine E. Goodman, Patricia J. Simner, Eili Y. Klein, Abida Q. Kazmi, Avinash Gadala, Clare Rock, Pranita D. Tamma, Sara E. Cosgrove, Lisa L. Maragakis, Aaron M. Milstone, for the CDC Prevention Epicenters Program, the CDC MIND-Healthcare Program
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 39 / Issue 12 / December 2018
- Published online by Cambridge University Press:
- 01 October 2018, pp. 1491-1493
- Print publication:
- December 2018
-
- Article
- Export citation
-
Using samples collected for VRE surveillance, we evaluated unit admission prevalence of carbapenem-resistant Enterobacteriaceae (CRE) perirectal colonization and whether CRE carriers (unknown to staff) were on contact precautions for other indications. CRE colonization at unit admission was infrequent (3.9%). Most CRE carriers were not on contact precautions, representing a reservoir for healthcare-associated CRE transmission.
Contributors
-
- By Mitchell Aboulafia, Frederick Adams, Marilyn McCord Adams, Robert M. Adams, Laird Addis, James W. Allard, David Allison, William P. Alston, Karl Ameriks, C. Anthony Anderson, David Leech Anderson, Lanier Anderson, Roger Ariew, David Armstrong, Denis G. Arnold, E. J. Ashworth, Margaret Atherton, Robin Attfield, Bruce Aune, Edward Wilson Averill, Jody Azzouni, Kent Bach, Andrew Bailey, Lynne Rudder Baker, Thomas R. Baldwin, Jon Barwise, George Bealer, William Bechtel, Lawrence C. Becker, Mark A. Bedau, Ernst Behler, José A. Benardete, Ermanno Bencivenga, Jan Berg, Michael Bergmann, Robert L. Bernasconi, Sven Bernecker, Bernard Berofsky, Rod Bertolet, Charles J. Beyer, Christian Beyer, Joseph Bien, Joseph Bien, Peg Birmingham, Ivan Boh, James Bohman, Daniel Bonevac, Laurence BonJour, William J. Bouwsma, Raymond D. Bradley, Myles Brand, Richard B. Brandt, Michael E. Bratman, Stephen E. Braude, Daniel Breazeale, Angela Breitenbach, Jason Bridges, David O. Brink, Gordon G. Brittan, Justin Broackes, Dan W. Brock, Aaron Bronfman, Jeffrey E. Brower, Bartosz Brozek, Anthony Brueckner, Jeffrey Bub, Lara Buchak, Otavio Bueno, Ann E. Bumpus, Robert W. Burch, John Burgess, Arthur W. Burks, Panayot Butchvarov, Robert E. Butts, Marina Bykova, Patrick Byrne, David Carr, Noël Carroll, Edward S. Casey, Victor Caston, Victor Caston, Albert Casullo, Robert L. Causey, Alan K. L. Chan, Ruth Chang, Deen K. Chatterjee, Andrew Chignell, Roderick M. Chisholm, Kelly J. Clark, E. J. Coffman, Robin Collins, Brian P. Copenhaver, John Corcoran, John Cottingham, Roger Crisp, Frederick J. Crosson, Antonio S. Cua, Phillip D. Cummins, Martin Curd, Adam Cureton, Andrew Cutrofello, Stephen Darwall, Paul Sheldon Davies, Wayne A. Davis, Timothy Joseph Day, Claudio de Almeida, Mario De Caro, Mario De Caro, John Deigh, C. F. Delaney, Daniel C. Dennett, Michael R. DePaul, Michael Detlefsen, Daniel Trent Devereux, Philip E. Devine, John M. Dillon, Martin C. Dillon, Robert DiSalle, Mary Domski, Alan Donagan, Paul Draper, Fred Dretske, Mircea Dumitru, Wilhelm Dupré, Gerald Dworkin, John Earman, Ellery Eells, Catherine Z. Elgin, Berent Enç, Ronald P. Endicott, Edward Erwin, John Etchemendy, C. Stephen Evans, Susan L. Feagin, Solomon Feferman, Richard Feldman, Arthur Fine, Maurice A. Finocchiaro, William FitzPatrick, Richard E. Flathman, Gvozden Flego, Richard Foley, Graeme Forbes, Rainer Forst, Malcolm R. Forster, Daniel Fouke, Patrick Francken, Samuel Freeman, Elizabeth Fricker, Miranda Fricker, Michael Friedman, Michael Fuerstein, Richard A. Fumerton, Alan Gabbey, Pieranna Garavaso, Daniel Garber, Jorge L. A. Garcia, Robert K. Garcia, Don Garrett, Philip Gasper, Gerald Gaus, Berys Gaut, Bernard Gert, Roger F. Gibson, Cody Gilmore, Carl Ginet, Alan H. Goldman, Alvin I. Goldman, Alfonso Gömez-Lobo, Lenn E. Goodman, Robert M. Gordon, Stefan Gosepath, Jorge J. E. Gracia, Daniel W. Graham, George A. Graham, Peter J. Graham, Richard E. Grandy, I. Grattan-Guinness, John Greco, Philip T. Grier, Nicholas Griffin, Nicholas Griffin, David A. Griffiths, Paul J. Griffiths, Stephen R. Grimm, Charles L. Griswold, Charles B. Guignon, Pete A. Y. Gunter, Dimitri Gutas, Gary Gutting, Paul Guyer, Kwame Gyekye, Oscar A. Haac, Raul Hakli, Raul Hakli, Michael Hallett, Edward C. Halper, Jean Hampton, R. James Hankinson, K. R. Hanley, Russell Hardin, Robert M. Harnish, William Harper, David Harrah, Kevin Hart, Ali Hasan, William Hasker, John Haugeland, Roger Hausheer, William Heald, Peter Heath, Richard Heck, John F. Heil, Vincent F. Hendricks, Stephen Hetherington, Francis Heylighen, Kathleen Marie Higgins, Risto Hilpinen, Harold T. Hodes, Joshua Hoffman, Alan Holland, Robert L. Holmes, Richard Holton, Brad W. Hooker, Terence E. Horgan, Tamara Horowitz, Paul Horwich, Vittorio Hösle, Paul Hoβfeld, Daniel Howard-Snyder, Frances Howard-Snyder, Anne Hudson, Deal W. Hudson, Carl A. Huffman, David L. Hull, Patricia Huntington, Thomas Hurka, Paul Hurley, Rosalind Hursthouse, Guillermo Hurtado, Ronald E. Hustwit, Sarah Hutton, Jonathan Jenkins Ichikawa, Harry A. Ide, David Ingram, Philip J. Ivanhoe, Alfred L. Ivry, Frank Jackson, Dale Jacquette, Joseph Jedwab, Richard Jeffrey, David Alan Johnson, Edward Johnson, Mark D. Jordan, Richard Joyce, Hwa Yol Jung, Robert Hillary Kane, Tomis Kapitan, Jacquelyn Ann K. Kegley, James A. Keller, Ralph Kennedy, Sergei Khoruzhii, Jaegwon Kim, Yersu Kim, Nathan L. King, Patricia Kitcher, Peter D. Klein, E. D. Klemke, Virginia Klenk, George L. Kline, Christian Klotz, Simo Knuuttila, Joseph J. Kockelmans, Konstantin Kolenda, Sebastian Tomasz Kołodziejczyk, Isaac Kramnick, Richard Kraut, Fred Kroon, Manfred Kuehn, Steven T. Kuhn, Henry E. Kyburg, John Lachs, Jennifer Lackey, Stephen E. Lahey, Andrea Lavazza, Thomas H. Leahey, Joo Heung Lee, Keith Lehrer, Dorothy Leland, Noah M. Lemos, Ernest LePore, Sarah-Jane Leslie, Isaac Levi, Andrew Levine, Alan E. Lewis, Daniel E. Little, Shu-hsien Liu, Shu-hsien Liu, Alan K. L. Chan, Brian Loar, Lawrence B. Lombard, John Longeway, Dominic McIver Lopes, Michael J. Loux, E. J. Lowe, Steven Luper, Eugene C. Luschei, William G. Lycan, David Lyons, David Macarthur, Danielle Macbeth, Scott MacDonald, Jacob L. Mackey, Louis H. Mackey, Penelope Mackie, Edward H. Madden, Penelope Maddy, G. B. Madison, Bernd Magnus, Pekka Mäkelä, Rudolf A. Makkreel, David Manley, William E. Mann (W.E.M.), Vladimir Marchenkov, Peter Markie, Jean-Pierre Marquis, Ausonio Marras, Mike W. Martin, A. P. Martinich, William L. McBride, David McCabe, Storrs McCall, Hugh J. McCann, Robert N. McCauley, John J. McDermott, Sarah McGrath, Ralph McInerny, Daniel J. McKaughan, Thomas McKay, Michael McKinsey, Brian P. McLaughlin, Ernan McMullin, Anthonie Meijers, Jack W. Meiland, William Jason Melanson, Alfred R. Mele, Joseph R. Mendola, Christopher Menzel, Michael J. Meyer, Christian B. Miller, David W. Miller, Peter Millican, Robert N. Minor, Phillip Mitsis, James A. Montmarquet, Michael S. Moore, Tim Moore, Benjamin Morison, Donald R. Morrison, Stephen J. Morse, Paul K. Moser, Alexander P. D. Mourelatos, Ian Mueller, James Bernard Murphy, Mark C. Murphy, Steven Nadler, Jan Narveson, Alan Nelson, Jerome Neu, Samuel Newlands, Kai Nielsen, Ilkka Niiniluoto, Carlos G. Noreña, Calvin G. Normore, David Fate Norton, Nikolaj Nottelmann, Donald Nute, David S. Oderberg, Steve Odin, Michael O’Rourke, Willard G. Oxtoby, Heinz Paetzold, George S. Pappas, Anthony J. Parel, Lydia Patton, R. P. Peerenboom, Francis Jeffry Pelletier, Adriaan T. Peperzak, Derk Pereboom, Jaroslav Peregrin, Glen Pettigrove, Philip Pettit, Edmund L. Pincoffs, Andrew Pinsent, Robert B. Pippin, Alvin Plantinga, Louis P. Pojman, Richard H. Popkin, John F. Post, Carl J. Posy, William J. Prior, Richard Purtill, Michael Quante, Philip L. Quinn, Philip L. Quinn, Elizabeth S. Radcliffe, Diana Raffman, Gerard Raulet, Stephen L. Read, Andrews Reath, Andrew Reisner, Nicholas Rescher, Henry S. Richardson, Robert C. Richardson, Thomas Ricketts, Wayne D. Riggs, Mark Roberts, Robert C. Roberts, Luke Robinson, Alexander Rosenberg, Gary Rosenkranz, Bernice Glatzer Rosenthal, Adina L. Roskies, William L. Rowe, T. M. Rudavsky, Michael Ruse, Bruce Russell, Lilly-Marlene Russow, Dan Ryder, R. M. Sainsbury, Joseph Salerno, Nathan Salmon, Wesley C. Salmon, Constantine Sandis, David H. Sanford, Marco Santambrogio, David Sapire, Ruth A. Saunders, Geoffrey Sayre-McCord, Charles Sayward, James P. Scanlan, Richard Schacht, Tamar Schapiro, Frederick F. Schmitt, Jerome B. Schneewind, Calvin O. Schrag, Alan D. Schrift, George F. Schumm, Jean-Loup Seban, David N. Sedley, Kenneth Seeskin, Krister Segerberg, Charlene Haddock Seigfried, Dennis M. Senchuk, James F. Sennett, William Lad Sessions, Stewart Shapiro, Tommie Shelby, Donald W. Sherburne, Christopher Shields, Roger A. Shiner, Sydney Shoemaker, Robert K. Shope, Kwong-loi Shun, Wilfried Sieg, A. John Simmons, Robert L. Simon, Marcus G. Singer, Georgette Sinkler, Walter Sinnott-Armstrong, Matti T. Sintonen, Lawrence Sklar, Brian Skyrms, Robert C. Sleigh, Michael Anthony Slote, Hans Sluga, Barry Smith, Michael Smith, Robin Smith, Robert Sokolowski, Robert C. Solomon, Marta Soniewicka, Philip Soper, Ernest Sosa, Nicholas Southwood, Paul Vincent Spade, T. L. S. Sprigge, Eric O. Springsted, George J. Stack, Rebecca Stangl, Jason Stanley, Florian Steinberger, Sören Stenlund, Christopher Stephens, James P. Sterba, Josef Stern, Matthias Steup, M. A. Stewart, Leopold Stubenberg, Edith Dudley Sulla, Frederick Suppe, Jere Paul Surber, David George Sussman, Sigrún Svavarsdóttir, Zeno G. Swijtink, Richard Swinburne, Charles C. Taliaferro, Robert B. Talisse, John Tasioulas, Paul Teller, Larry S. Temkin, Mark Textor, H. S. Thayer, Peter Thielke, Alan Thomas, Amie L. Thomasson, Katherine Thomson-Jones, Joshua C. Thurow, Vzalerie Tiberius, Terrence N. Tice, Paul Tidman, Mark C. Timmons, William Tolhurst, James E. Tomberlin, Rosemarie Tong, Lawrence Torcello, Kelly Trogdon, J. D. Trout, Robert E. Tully, Raimo Tuomela, John Turri, Martin M. Tweedale, Thomas Uebel, Jennifer Uleman, James Van Cleve, Harry van der Linden, Peter van Inwagen, Bryan W. Van Norden, René van Woudenberg, Donald Phillip Verene, Samantha Vice, Thomas Vinci, Donald Wayne Viney, Barbara Von Eckardt, Peter B. M. Vranas, Steven J. Wagner, William J. Wainwright, Paul E. Walker, Robert E. Wall, Craig Walton, Douglas Walton, Eric Watkins, Richard A. Watson, Michael V. Wedin, Rudolph H. Weingartner, Paul Weirich, Paul J. Weithman, Carl Wellman, Howard Wettstein, Samuel C. Wheeler, Stephen A. White, Jennifer Whiting, Edward R. Wierenga, Michael Williams, Fred Wilson, W. Kent Wilson, Kenneth P. Winkler, John F. Wippel, Jan Woleński, Allan B. Wolter, Nicholas P. Wolterstorff, Rega Wood, W. Jay Wood, Paul Woodruff, Alison Wylie, Gideon Yaffe, Takashi Yagisawa, Yutaka Yamamoto, Keith E. Yandell, Xiaomei Yang, Dean Zimmerman, Günter Zoller, Catherine Zuckert, Michael Zuckert, Jack A. Zupko (J.A.Z.)
- Edited by Robert Audi, University of Notre Dame, Indiana
-
- Book:
- The Cambridge Dictionary of Philosophy
- Published online:
- 05 August 2015
- Print publication:
- 27 April 2015, pp ix-xxx
-
- Chapter
- Export citation
Contributors
-
- By Sherese Ali, Danielle Molinari Andrade, Elinor Ben-Menachem, Weerawadee Chandranipapongse, Pamela Crawford, Anne Davis, Carin Dove, Nancy Foldvary-Schaefer, Elizabeth E. Gerard, Cristina Y. Go, Cynthia L. Harden, Dini Hui, Shinya Ito, Jaromir Janousek, Nathalie Jette, Pavel Klein, A. Gabriela Lizama, Kristi A. McIntosh, Georgia Montouris, Brian J. Murray, Ori Nevo, Eugene Ng, Alison M. Pack, Sima Indubhai Patel, Page B. Pennell, Kalliopi A. Petropoulou, Mark Quigg, Alessandra Scaparrotta, Marianna Sebastiani, Patricia Osborne Shafer, O. Carter Snead, Diane T. Sundstrom, Alberto Verrotti, Carla Verrotti, Jonathan H. Waters, Fatima Zahir
- Edited by Esther Bui, Autumn M. Klein
-
- Book:
- Women with Epilepsy
- Published online:
- 05 August 2014
- Print publication:
- 31 July 2014, pp vii-x
-
- Chapter
- Export citation
List of contributors
-
- By Bjarne F. Alsbjoern, Caroline M. Apovian, Danny Collins, Roland N. Dickerson, Timothy Eden, Peter Faber, Andrew J. Ferguson, David C. Frankenfield, Dympna Gallagher, Maria Gabriella Gentile, Wilson I. Gonsalves, Andrew M. Hetreed, Michael H. Hooper, Jan O. Jansen, Aminah Jatoi, Ying Ji, Ilya Kagan, Andrew J. Kerwin, Dong Wook Kim, Andrew A. Klein, Alistair Lee, Shaul Lev, Peter K. Linden, Paul E. Marik, Robert Martindale, Peter McCanny, Paolo Merlani, Shay Nanthakumaran, Michael S. Nussbaum, Andreas Perren, Carla Prado, Jean-Charles Preiser, Minha Rajput-Ray, Sumantra Ray, Nils Siegenthaler, Mario Siervo, Jonathan A. Silversides, Pierre Singer, John A. Tayek, Euan Thomson, Krista L. Turner, Malissa Warren, Stephen T. Webb, Patricia Wiesen
- Edited by Peter Faber, Mario Siervo, University of Newcastle upon Tyne
-
- Book:
- Nutrition in Critical Care
- Published online:
- 05 April 2014
- Print publication:
- 06 March 2014, pp viii-xii
-
- Chapter
- Export citation
Gametogenic cycle of the tropical vermetids Eualetes tulipa and Dendropoma corrodens (Mollusca: Caenogastropoda: Vermetidae)
- Patricia Miloslavich, Eduardo Klein, Pablo Penchaszadeh
-
- Journal:
- Journal of the Marine Biological Association of the United Kingdom / Volume 90 / Issue 3 / May 2010
- Published online by Cambridge University Press:
- 09 December 2009, pp. 509-518
-
- Article
- Export citation
-
The population density, annual gametogenic cycle, and size at sexual maturity of two vermetid species, Eualetes tulipa (invasive) and Dendropoma corrodens was studied in the southern Caribbean at the Planta Centro power plant intake channel and at Punta Mayorquina, Morrocoy National Park, respectively. Minimal size of mature females of E. tulipa and D. corrodens was 5.0 and 0.7 cm in body length respectively. The gonad represented between 44 to 47% of total body length, while it represented between 15 to 18% of total body volume (for both males and females). Gonad volume was significantly related to total body volume. A significant quadratic relationship between the number of capsules and female body volume was obtained for E. tulipa, indicating that females measuring 6–10 cm in body length are those that have the highest number of egg capsules. Females larger than 11 cm have a lower fecundity in terms of brooded capsules. Gonad sections of males and females of both species showed that several gametogenesis stages are simultaneous within the same individual. In the female, germ cells, oogoniums and primary oocytes with yolk granules were observed simultaneously. In the male, the spermatogonium, primary and secondary spermatocytes, spermatids and sperm cells were also observed within one gonad. The same pattern was observed throughout the year, showing no maturation/resting period or annual cycle. The area covered by D. corrodens was about 700 m2 with a mean density of 13,000 ind/m2. The area covered by the invasive E. tulipa was at least about 1000 m2, with a density of 27,000 to 29,000 ind/m2 in the first 3 m of depth. A follow up of the E. tulipa population showed that its density is increasing in time and has doubled in 20 years. This population increment could be related to an increase in organic suspended matter as evidenced in the region.
Interpreting the unexpected: the case of AIDS policy making in Britain
- Patricia Day, Rudolf Klein
-
- Journal:
- Journal of Public Policy / Volume 9 / Issue 3 / July 1989
- Published online by Cambridge University Press:
- 28 November 2008, pp. 337-353
-
- Article
- Export citation
-
This paper analyses the reactions of a government faced with an unpredictable and unexpected crisis with possible catastrophic long-term effects: the AIDS epidemic in the United Kingdom in the 1980s. First, the AIDS epidemic is defined as a case study of government forced to cope with uncertainty, moral ambiguity and the knowledge that there are no solutions, only ways of limiting the damage. Second, it examines the evolution of policy of British ministers, who initially preferred to ignore evidence of AIDS but were forced to act by signals threatening a popular backlash. They did so by creating a programme of action based on the advice and values of the medical profession and public health experts. The conclusion argues that this kind of policy response may be generalisable. When societies are faced with problems that do not appear to be soluble but which may imperil social cohesion they seek to create an elite consensus to treat them as technical matters, so insulating the policy process from possible disruptive populist pressures.